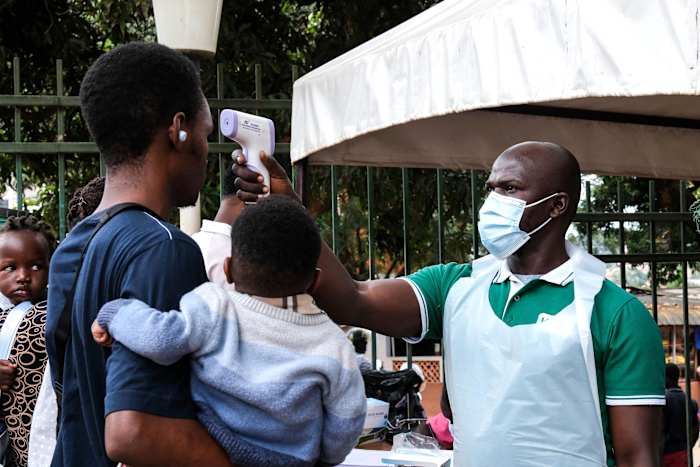
The World Health Organization just declared the Ebola outbreak spreading across the Democratic Republic of the Congo and Uganda a Public Health Emergency of International Concern. If this sounds like a familiar administrative ritual, that is because the global health apparatus has conditioned us to view these announcements as bureaucratic paperwork. But beneath the official jargon lies a far more volatile reality. This is not a standard flare-up.
The current outbreak is driven by the Bundibugyo virus, a rare and clinically elusive strain of Ebola that has evaded the medical breakthroughs of the last decade. There are no approved vaccines for this specific species. The highly publicized stockpiles of Ervebo and Sabdeno vaccines that halted previous epidemics are utterly useless here, leaving front-line responders defensively hollowed out. Compounding the biological threat is a catastrophic geographic reality: the epicenter is a high-traffic gold mining zone in the DRC’s conflict-torn Ituri province, and infected travelers have already carried the virus into the capital cities of Kampala and Kinshasa.
http://googleusercontent.com/image_content/191
By the time the global community parsed the initial data, the structural failures of the regional containment network had already been exposed.
The Illusion of Preparedness
For years, global health institutions pointed to the eastern Congo as proof that modern medicine had tamed Ebola. We were told that rapid diagnostic infrastructure, experimental monoclonal antibodies, and ring-vaccination protocols had transformed a historical terror into a manageable endemic risk.
That narrative has collapsed. The international community made the mistake of treating Ebola as a monolith.
The vast majority of research, funding, and pharmaceutical development over the past ten years targeted a single species: Orthoebolavirus zairense, commonly known as the Zaire strain. Because the Zaire variant caused the horrific West African epidemic of 2014-2016 and subsequent major outbreaks in the DRC, it sucked all the oxygen out of the room. The therapeutic weapons we built—the Merck and Johnson & Johnson vaccines, alongside highly effective monoclonal antibody treatments—were engineered specifically for Zaire.
The Bundibugyo strain, first identified in western Uganda in 2007, possesses a completely different genetic architecture.
Ebola Strains & Vaccine Availability (2026)
┌───────────────────┬──────────────────────────┐
│ Species / Strain │ Approved Vaccine Status │
├───────────────────┼──────────────────────────┤
│ Zaire │ Fully Available (Ervebo) │
│ Sudan │ Experimental Only │
│ Bundibugyo │ NONE │
└───────────────────┴──────────────────────────┘
Because Bundibugyo does not respond to Zaire-targeted therapeutics, clinicians in Ituri are forced back into the medical stone age. They are relying almost exclusively on supportive care: aggressive intravenous rehydration, electrolyte management, and blood transfusions. While Bundibugyo historically carries a lower mortality rate than Zaire—hovering around 30 to 45 percent rather than the catastrophic 70 to 90 percent—the lack of targeted medical interventions means patient outcomes depend entirely on the speed and quality of basic hospital care. In a collapsed health system, that is a losing bet.
A Perfect Storm in the Mining Fields
The outbreak originated in the Mongbwalu health zone, an anarchic hub of artisanal gold mining in the Ituri province. To understand why this environment is a public health nightmare, one must understand the economic geography of the region.
Artisanal mines are populated by an incredibly fluid, transient workforce. Thousands of young men and their families move constantly between makeshift settlements, driven by the fluctuating price of gold and the movement of armed militias. There are no formal employee rosters. There is no central HR database.
When an individual falls ill in an artisanal mining camp, they do not quietly quarantine in a modern isolation ward. They move.
As patients in Mongbwalu began deteriorating, they fled the squalor of the camps to seek care or family support in the larger regional hubs of Rwampara and Bunia. This internal migration transformed a localized cluster into an active multi-zone network of community transmission. Because the early symptoms of Ebola—sudden fever, intense muscle pain, fatigue, and headaches—mimic malaria and typhoid, these mobile laborers mingled with local populations and entered general health clinics completely undetected.
By the time the National Institute of Biomedical Research in Kinshasa confirmed Bundibugyo from local samples, the virus had already used the region's transport arteries to leap across borders.
A single laboratory-confirmed case emerged in Kinshasa, carried by an individual returning from the eastern goldfields. Concurrently, across the border in Uganda, two separate travelers from the DRC arrived in the capital city of Kampala. Both tested positive for the virus; one has already died. The WHO took pains to note that these two cases in Kampala share no apparent epidemiological link other than their point of origin in the Congo. This detail is crucial. It indicates that the volume of infected individuals moving out of the primary hot zone is high enough to produce multiple, independent exportations across international boundaries.
The Ghost of Conflict
Conducting contact tracing in a stable environment is difficult. Doing it in Ituri is nearly impossible.
The province is currently a patchwork of active battlefields. Islamic State-backed militants and local ethnic self-defense factions carry out routine, brutal raids on villages and transport routes. This systemic insecurity does more than terrorize the civilian population; it completely paralyzes rapid response teams.
Epidemiologists cannot safely enter a village to trace the contacts of a deceased miner if that village is under threat of an armed assault. Supplying personal protective gear, clean water, and testing reagents requires secure logistical corridors that simply do not exist. When health workers cannot safely operate, the virus gains a cloaking device.
Local testimony gathered from the provincial capital of Bunia reveals that community panic is outpacing the international response. Residents report that families are burying multiple people a day without any oversight from trained burial teams. In an Ebola outbreak, the corpse of a victim is at its most infectious stage. Traditional funeral rites that involve washing and touching the deceased act as hyper-spreading events.
Without secure access to these communities to enforce safe burials and educate grieving families, the formal case numbers published by the WHO—fewer than ten laboratory-confirmed cases against roughly 250 suspected infections—represent an extreme undercount. The official statistics are merely a snapshot of what is happening near the main roads; the true scale of the epidemic is buried deep in the inaccessible interior.
The Flawed Logic of Border Closures
Whenever a highly lethal pathogen hits the headlines, the immediate political reflex in Western capitals and neighboring nations is to demand the closure of international borders. The WHO specifically advised against travel or trade restrictions in its emergency declaration. This is not out of a sense of diplomatic politeness, but rather a calculated strategy to prevent the outbreak from spinning completely out of control.
History has repeatedly demonstrated that closing formal border checkpoints does not stop desperate people from moving; it merely drives them into the shadows.
The border between the eastern DRC and western Uganda is a porous, artificial line cutting through thick forests and long-standing tribal territories. Thousands of people cross it daily via informal "panya" routes—dirt paths through the bush—to trade goods, visit family, or flee violence. If Uganda or the DRC seals the official crossings, travelers showing early symptoms of illness will simply bypass medical screening stations entirely.
Formal Border Post (Screening) ──> Temperature Checked ──> Isolated if Symptomatic
Informal Path (Closure Reflex) ──> No Screening ──> Enters Population Secretly
Instead of stopping the virus, aggressive border restrictions actively blind public health officials. It forces infected individuals to hide their illnesses, avoid formal hospitals, and rely on informal, underground care where infection control is nonexistent.
The real solution is far more tedious and expensive: keeping borders open while massively reinforcing visible, non-punitive health screening at every major transit junction. But that requires sustained funding and international solidarity, two commodities that usually dry up once the initial wave of media panic subsides.
Breaking the Cycle
The declaration of a global health emergency is a call for funding, but money alone will not solve a structural crisis rooted in institutional neglect. The international community must abandon the reactive, single-strain strategy that left us defenseless against the Bundibugyo virus.
We cannot afford to treat vaccine development as a commercial enterprise that only responds to the most profitable or high-profile threats.
Developing pan-Ebola therapeutics that target the shared biological mechanisms of all six known strains must become an absolute priority for global health security. Until that shift occurs, the front-line health workers in Bunia, Mongbwalu, and Kampala will continue fighting a 21st-century bio-hazard with little more than plastic aprons, bleach buckets, and hope. The virus has already demonstrated its ability to travel from an isolated mining pit to two African capitals in a matter of days. Expecting it to stop there is a luxury the world cannot afford.